Woman Dies From Rare Brain Disorder Following Second Pfizer Shot; Husband Calls Us "Guinea Pigs"
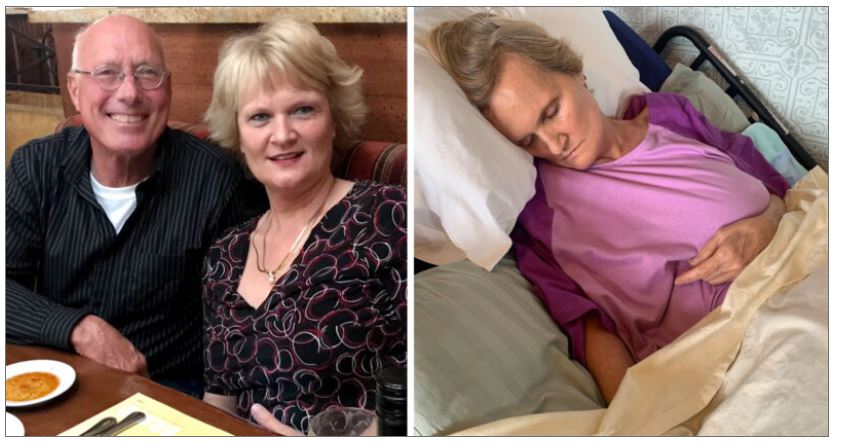
Jennifer Deason Sprague, a healthy 60-year-old woman from Missouri, died Feb. 21, five months after receiving her second dose of Pfizer’s COVID-19 vaccine.
Jennifer died from Creutzfeldt-Jakob Disease (CJD), a fatal degenerative brain disorder.
In an exclusive interview with The Defender, Richard Sprague said his wife received the first dose of Pfizer on Aug. 29, 2021, and her second dose on Sept. 21, 2021.
Although he remained unvaccinated, Sprague said his wife got the vaccine because she worked for the Perkins Restaurant Corporation, which required employees to get the shot.
“I told her to just lie about it and if they asked for a vaccination card, then she should ask them to make everyone show proof they had the shot,†Sprague said. “She felt bad lying about it, so she went ahead and got it.â€
Four days after the second dose,
Jennifer experienced her first episode of a “sudden strange event she
couldn’t explain,†while she and her husband were at a dinner theater.
Sprague said:
“We had just finished our meal and were just visiting. All at once, she said, ‘There is something wrong. Please take me home now. I don’t know what it is and I cannot explain it.’ So we missed the theater and went straight home.â€
The following week Jennifer called her doctor and asked if the episode she experienced could be related to the COVID vaccine.
“The doctor said if it was the shot, she would have known it after a couple of hours, not a couple of days,†Sprague said.
Jennifer started having more episodes and her left hand and side began to tremble. On Oct. 13, 2021, Jennifer went back to the doctor, who prescribed Xanax for anxiety.
Over the next few weeks, her symptoms worsened and her left side began to feel heavier than her right side, Sprague said. This continued throughout November and December. Jennifer’s doctor instructed her to stay on the Xanax because he thought it was anxiety.
Jennifer experienced another episode of the “events she couldn’t explain†on Dec. 24, 2021, only this time it was worse, Sprague said. She told everyone she needed to go home and apologized.
Later that evening, Sprague took his
wife to the ER, where physicians treated her for anxiety and recommended
pills she could take to “get her through the night.†The doctors could
find nothing wrong with her, Sprague said.
The next morning, Jennifer went
to work at Perkins, as all employees were required to work on Christmas
day. But by 10 a.m., Richard got a call to pick up his wife.
“She had a very bad episode at work,†Sprague explained. “She couldn’t hold a tray or pour coffee.â€
Sprague found a new doctor. At
Jennifer’s appointment on Jan. 5, the physician said she was being
over-medicated and stopped everything cold turkey, thinking this would
resolve her symptoms, Sprague said.
A follow-up was scheduled for Feb. 10, but Sprague took Jennifer back to the doctor at the end of January because her symptoms were more severe.
Sprague explained:
“By this time, I’m having to tow her along when we walk. We would go to the mall and walk laps so she was in shape when she would return to work, but around January 23, to look at my wife — if this is Xanax withdrawal I felt I needed someone to encourage me.
“She was having a hard time dressing herself. It would take her two hours to get focused in the morning, and her brain fog was bad. She would lose her train of thought. After 30 minutes or so I’d walk in the bathroom and ask if she was okay and the shower would be cold again. At the time, we laughed about it.â€
“When I took Jennifer back to the doctor, they took one look at her and knew something was going on,†Sprague said. Doctors performed blood work and MRIs, but the results came back normal.
“They recommended a neurologist — because something didn’t look quite right — and a psychiatrist to see if it was psychological, which scared Jennifer because she said she wasn’t crazy,†Sprague said. “If this was Xanax withdrawal this thing would be turning around any day.â€
Sprague said:
“Early that evening something happened in her head. She did not like the neurologist because he wanted her to see the psychiatrist and she started repeating herself over and over: ‘This guy thinks I’m crazy. This guy thinks I’m crazy.’ She started stumbling around. She stumbled trying to get in the car. I called my son to help me and we took her straight home.â€
After they arrived home, two of Sprague’s children — an RN and a chemist — came over. They persuaded Jennifer to go back to the ER.
“Doctors immediately did another MRI and admitted her around January 30,†Sprague said.
At the time, Jennifer was still able to sit up and walk independently.
“I didn’t know it at the time, but the neurologist had read the MRI and saw a significant change on the right side of her brain and suspected CJD,†Sprague said. “They didn’t tell me because they wanted to rule out everything else.â€
Doctors did more scans of Jennifer’s brain and entire body to rule out infections and cancer. “They said she was a 60-year-old in a 40-year-old’s body,†Sprague said.
At the end of the week, Jennifer’s doctors said they needed to perform a spinal tap, but by this time, she was unable to get out of bed by herself.
Sprague said:
“In one
week she started regressing so fast it was unbelievable. She was fogged,
having a hard time, was seeing snakes on the wall — like she had
dementia — and it would only last about three days until that part of
the brain was gone. But she never forgot who I was. She always
remembered who I was.â€
The spinal tap confirmed Jennifer had CJD, a prion disease. A study
published last year in Microbiology & Infectious Diseases found a
potential link between Pfizer’s COVID vaccine and prion disease in
humans.
Comments
There are 0 comments on this post